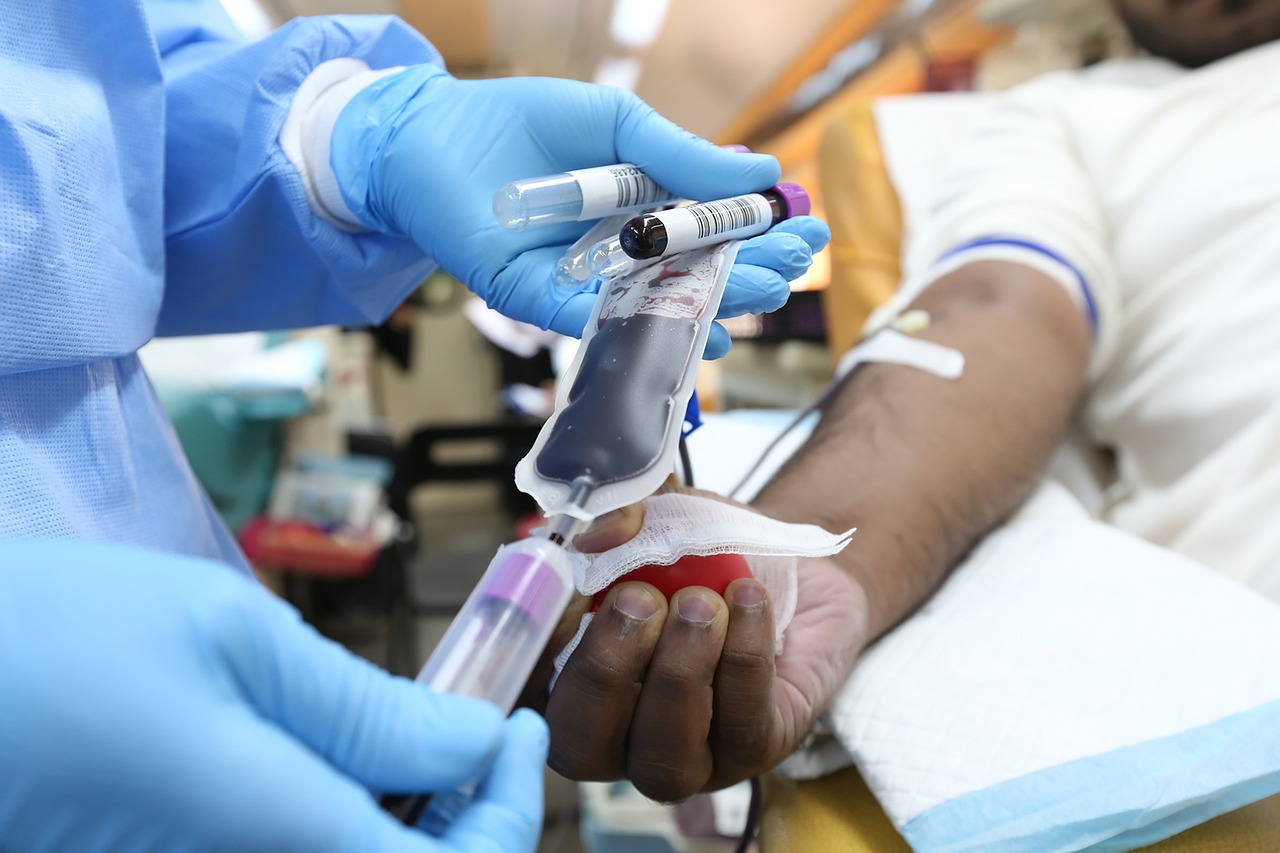
Curious how Absorbed Anti-A1 is prepared? Have there been countless lives saved by blood transfusions? Mismatches between a patient’s blood type? Transfusion of blood can cause serious complications, including death. In some cases, anti-A1 antibodies are used to prevent these issues. How are these antibodies made?
The presence or absence of certain proteins, called antigens, on the surface of red blood cells determine a blood type. Blood types include A, B, AB, and O. Type A blood cells can contain two main antigens: A and A1. Transfusions can be complicated if the recipient’s immune system recognizes and attacks the A1 antigen as foreign. Anti-A1 antibodies can neutralize the A1 antigen to prevent this. The purpose of this article is to explain how these antibodies are made.
What are anti-A1 antibodies?
Anti-A1 antibodies bind to the A1 antigen on red blood cells and recognize it. Your immune system makes antibodies when exposed to the A1 antigen through blood transfusions or pregnancy. Some people don’t produce enough anti-A1 antibodies naturally, so they need to get them from somewhere else.
How are anti-A1 antibodies prepared?
Anti-A1 antibodies can be prepared in several ways. Getting blood from people who naturally produce anti-A1 antibodies is a common method. Antibodies can be isolated from this blood, known as hyperimmune anti-A1 serum. First, the serum is tested for safety. Then, it’s purified.
Genetic engineering is another way to make anti-A1 antibodies. Scientists can make monoclonal antibodies, which produce the desired antibodies in large quantities. Antibodies can be made on a large scale in bioreactors.
How are absorbed anti-A1 antibodies prepared?
Absorbed anti-A1 antibodies are anti-A1 antibodies that have been treated to remove any unwanted antibodies that could cause adverse reactions. The hyperimmune anti-A1 serum is mixed with red blood cells without the A1 antigen to make absorbed anti-A1 antibodies. Antibodies can then bind to other antigens on red blood cells, leaving only anti-A1 antibodies behind. Transfusions can then be done with these purified antibodies.
What have absorbed iron supplements?
An absorbable iron supplement is a type of dietary supplement that contains iron that’s easy to absorb. Usually, these supplements treat iron deficiency anemia and other conditions caused by low iron levels. Absorbable iron supplements are designed to be gentle on your stomach and increase iron levels effectively, unlike other iron supplements that can cause digestive issues.
How are absorbed iron supplements prepared?
Iron supplements can be prepared in several ways. Chelation is a way to improve mineral absorption by binding it to an organic molecule. Chelates are made by combining iron with amino acids, peptides, or other organic molecules.
Encapsulation is another way to get absorbed iron supplements. Iron is coated with a protective layer during this process to prevent it from reacting with other compounds. Iron can then pass through the stomach and into the small intestine, where it can be absorbed.
How does iron absorption from supplements work?
They have absorbed iron supplements by increasing iron levels, which can help red blood cell production. These supplements contain iron easily absorbed by the body and can quickly boost iron levels. Iron deficiency anemia symptoms like fatigue and weakness can be relieved this way.
What is stem cell therapy?
Stem cell therapy uses stem cells to repair or replace damaged cells or tissues. Stem cells can become many different types of cells, like blood, nerve, and muscle cells. In addition, they can self-renew, meaning they can divide and make more stem cells.
Embryonic stem cells, adult stem cells, and induced pluripotent stem cells can all be used for therapy. The embryonic stem cells can develop into any cell in the body. Adult stem cells can develop into different types of cells in different tissues. Adult cells can be reprogrammed to act like embryonic stem cells to make induced pluripotent stem cells.
What can stem cell therapy do for autoimmune diseases?
Stem cell therapy can treat autoimmune diseases by modulating the immune system and reducing inflammation. Mesenchymal stem cells (MSCs) are a type of adult stem cell found in bone marrow, adipose tissue, and other tissues. MSCs have immunomodulatory effects and can suppress immune cells that cause autoimmune diseases.
Hematopoietic stem cell transplantation (HSCT) involves replacing a patient’s immune system with stem cells from a donor. As a result, the new immune system can re-educate the immune cells to recognize healthy cells and tissues as “self.”
Are stem cell therapies for autoimmune diseases beneficial or risky?
Stem cell therapy may improve symptom control, disease progression, and quality of life in people with autoimmune diseases. Several studies have shown that stem cell therapy can be effective for certain autoimmune conditions, such as multiple and systemic sclerosis.
It should also be noted, however, that stem cell therapy does have some potential risks, such as infection, bleeding, and allergic reactions.
Additionally, there is a risk of graft-versus-host disease (GVHD) with HSCT, in which the donor’s immune cells attack the patient’s healthy cells and tissues due to the transplant. To determine the safety and efficacy of stem cell therapy for treating autoimmune diseases, further research is needed to determine the long-term effects of stem cell therapy.
Summary
A promising new treatment option for people suffering from autoimmune diseases is called stem cell therapy. Decrease inflammation and modulate the immune system, and stem cell therapy may offer a way to manage symptoms and slow disease progression by modulating the immune system. Despite these benefits and risks, it is important to weigh the potential benefits and risks of stem cell therapy with a healthcare provider, participate in clinical trials, or receive treatment from a qualified healthcare provider.